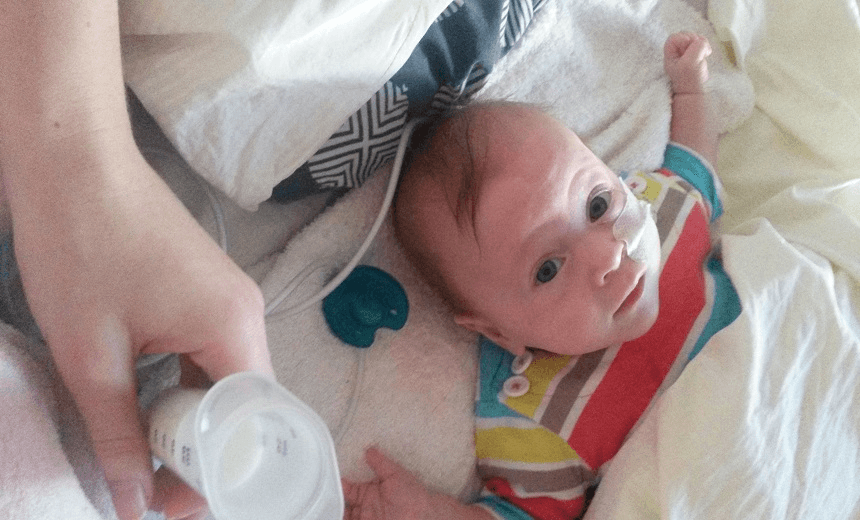
What would you do if your baby couldn’t eat? Jenn Gilbert shares her family’s story of naso-gastric tube feeding baby Ada.
When I was pregnant with my first child, I had the usual first-timer anxieties. Would I ever sleep again? Would my baby cry a lot? Would my body ever be the same?
But there were a few things I knew would be true. I would nourish my baby – by bottle or breast. Being able to feed your child is a given, right?
Wrong.
From the very beginning, I couldn’t nourish my daughter.
When she was born at 30 weeks because of my placenta failing, she was already small at just over a kilogram.
As with all 30-weekers she was looked after in the Neonatal Intensive Care Unit (NICU). She was fed by naso-gastric (NG) tube and I was told it would only be a matter of time until she would transition from the tube to the breast or bottle.
In order to “escape” the NICU, babies must be able to maintain their own temperature, breathe on their own, be gaining weight, and be able to feed. Ada slowly ticked off each milestone except for the last one.
Eventually we were told we could take her home with her NG tube and wean her there, over a week or two. I jumped at the opportunity to take her home. It had been seven long weeks in the NICU, and I was dying to be able to mother her myself, rather than being a ‘bystander’ mother while nurses did their thing.
I trusted the professionals that it would only be a week or two and the tube would be gone.
Again, I was wrong.
At the beginning we were visited by Homecare nurses every day or two. They assured me that it wouldn’t be long until she was feeding. Once she hit 3kg she would feed. Or, once she hit her due date. OK, maybe once she hit 4kg. Oh, no, maybe when she starts solids?
After a while these assurances started to wear thin.
At the beginning, I was still desperate to try and breastfeed her. So each feed went like this:
I put her to the breast where she would play around for a minute or two.
I would pray, beg, and cry: Come on baby, feed!
After this inevitably failed, I topped her up with a bottle. Just like breastfeeding it was a fruitless effort.
After this (by which time I was usually feeling quite low), I would tube feed her the majority of her milk.
Once I had done this, I would pump breastmilk, then clean all the equipment.
This whole soul destroying cycle took about two hours. My daughter needed to be fed every three hours.
It left very little time for any other form of mothering – or rest. I felt like a hamster on a wheel and I hit some very dark places, especially in the long nights.
After about a month or two of this, I gave up on my attempts to breastfeed her. I no longer cared about that, and I could no longer sustain the ‘boob-bottle-tube-pump’ routine.
At this time I also realised that her feeding issues weren’t just going to resolve themselves. I reached breaking point and started to fight for help. I insisted on a speech language therapist and dietician referral. I started researching online and joined an amazing tube feeding NZ Facebook group.
When Ada finally got assessed formally by a speech language therapist the news was dire. I was told that Ada had no suck/swallow/breathe skill and it could be months, a year, or even longer, until she would be tube-free. I was devastated but also felt a sense of peace. I had known something was going on and it was a relief to finally have a diagnosis. With a diagnosis we could move forward with a realistic plan, instead of losing hope at every feed.
As the months went by, it became easier than it had been at the start. Tube feeding was our new normal and we were waiting to see when Ada would show us she was ready to be tube-free. Only very occasionally would I feel the pain from our journey.
I vividly remember breaking down once in a SPACE group as other mothers effortlessly (it seemed!) breast and bottle fed their babies.
Over the months, the NG tubes would come out and we learned to reinsert them. This involved holding Ada down while she screamed and looked at me with a pained look in her eyes. I absolutely hated reinserting Ada’s tube. Once a friend accidentally knocked her tube out (through no fault of their own) and I had to leave the room to hide my rage and tears that I would have to insert the tube again because of their foolishness.
At around eight months old, two things happened. I decided to stop pumping. It was so draining (literally!) and I wanted to spend more time with Ada, rather than the pump. This wasn’t an easy decision, as it felt like a symbol of my failure as a mother and nourisher. However an amazing La Leche League leader spent an hour with me on the phome and helped me come to peace with my decision to stop pumping.
Also at this time, the speech language therapist suggested we trial a ‘tube wean’ for a few days to see if we could get her to take a bottle.
The tube came out and I recorded every millilitre that she drank. I still have the notebook. It’s sad reading.
8am- 20ml.
8.15am- 5ml.
9am- 10ml….And so on.
By the end of day three she had stopped weeing, and was dropping weight. The tube wean attempt was aborted. She wasn’t ready yet.
I started researching overseas weaning programs. I felt an urgency to wean her from the tube before it became a permanent fixture. New Zealand has a tube weaning program at Starship (funded by New World) which I applied for but she was too young. I got a private speech language therapist to come in, in case our public therapist had missed anything, but there was nothing new. There was really nothing we could do except wait for her to be ready.
At around 10 months old we attempted another tube wean. This time…she was ready!
She took small amounts of milk over the day, 50 or 60ml at a time. Occasionally 80.
We weighed her every second day and she was gaining weight. She was doing it! She was feeding! After about a week, the speech language therapist declared her tube-free! And about a month after that I ceremoniously threw out or gave away all of our remaining tube feeding equipment.
It wasn’t smooth sailing after she was tube-free. Ada’s weight was, and still is, a concern. She was under the care of many specialists until she was around three. Ada still eats very little but now at three-and-a-half she eats a variety of food and enjoys eating to make her “big and strong”.
I couldn’t be prouder of Ada and how far she has come since those early days. We were fortunate to get support and care both from medical professionals, but especially from other parents who had been there, done that.
Jenn is a mum of two preschoolers and lives with her kids and husband in Lower Hutt. She is an occasional writer, a part time NZSL interpreter and a full time mum and coffee drinker. If you would like to learn more about tube feeding, or support families going through this process, visit TubeWeanNZ.
Follow the Spinoff Parents on Facebook and Twitter.